How to sell employee benefits during a recession
As the COVID-19 pandemic continues to impact the economy, companies have struggled to find their way, instituting layoffs, furloughs, and hiring and spending freezes in the process. This has left employers, benefit brokers and benefit administrators wondering how to proceed.
Until recently, employers had focused primarily on attracting and retaining talent through rich benefits packages. As a result, brokers and benefit administrators emphasized added value when selling benefits. With the economy in a recession, however, the focus has shifted dramatically to cost savings. Now benefit administrators need to know how to sell employee benefits when purse strings are tight.
The following framework will provide solutions and strategies for fine-tuning your message in the current environment.
Craft the value proposition
Though the solution or offer to employers may seem inherently enticing and like a sure-fire win, brokers and benefit administrators would do well to approach the value proposition in a more thoughtful way.
1. Identify the employer’s key concern.
As tempting as it may be to start with the solution, you’ll likely see more traction by flipping the script. Begin by identifying the employer’s key concern. Right now, for example, their key concern may be a decreased HR budget and challenges determining how to deliver comprehensive benefits plans for less. Acknowledge this concern.
2. Talk about the alternative.
Talk about how others have tried to address this challenge but have failed. You could look at traditional PPO models and the cost burden those often place on corporations through premium cost-sharing and plan-year price hikes.
3. Demonstrate the solution.
At this point, you can step in and show the better approach. Beyond simply talking about the right solution, you must demonstrate exactly how the solution will work. Talk about cost savings in real numbers, and show how you got those numbers. Help employers see the real value and its attainability.
Focus on cost-saving benefit options
Benefit administrators who sell consumer-directed healthcare (CDH) have an opportunity to sell employee benefits to brokers and employers by pushing for alternative plan design and funding models that save money.
1. Optimize plan design with HDHPs
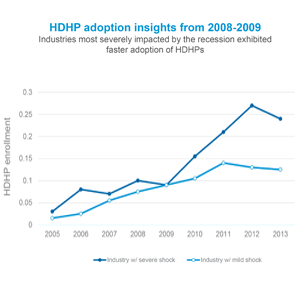
According to a study in the Journal of Health Economics, during the Great Recession of 2008, “the enrollment rate of high deductible health plans (HDHPs) among workers covered by employer-sponsored health benefits increased more among firms in industries that experienced severe recession shocks.”
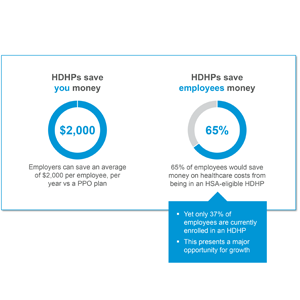
As employers deal with similar shockwaves from the pandemic-induced recession, the time is ideal for benefit administrators to push for HDHP adoption. HDHPs not only save employers money (up to $2,000 per employee per month, according to an analysis by Alegeus) but also pay off for consumers. Analysis of enrollment data suggests that more than 65% of consumers would save money with an HSA-qualified HDHP versus traditional PPO coverage.
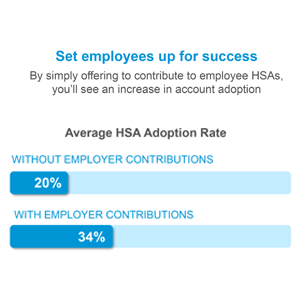
For several reasons – such as low fluency or hesitation to change from plans they already know – only 37% of the population is currently enrolled in HDHP plans. This presents a significant opportunity for brokers and benefit administrators to capture the market. Employers that don’t currently offer HDHPs and HSAs may now feel the extra push to shift their benefit plan designs, and those that already do may be open to refining their strategies – such as seeding employee accounts – to boost participation.
2. Consider offering ICHRAs
During an already complicated time for many businesses, individual coverage health reimbursement arrangements (ICHRAs) can offer a simplified approach to health benefits. ICHRAs, which became active in January 2020, allow employers to contribute funds to an employee’s account to cover medical care expenses up to a maximum dollar amount. This money can go toward the premium on a marketplace health insurance plan or pay for out-of-pocket medical costs. An analysis by Aite Group suggests that ICHRAs offer “a valuable value proposition for employers with tighter budgets” that’s worth benefit administrators exploring. Funding ICHRAs not only removes a layer of complexity from the benefits process, but also helps control costs. Employers can design ICHRAs and set their budget, tax-free, while avoiding surprise cost increases for groups plans that occur some years. ICHRAs may be particularly appealing to small businesses, which were hardest hit by COVID-19. Even before the pandemic, small businesses made up 78% of companies signing up for ICHRAs, owing to the plan’s flexibility and relative affordability.
For all the advantages for employers, ICHRAs also provide significant value to employees. Individuals can find the health coverage that is right for their unique needs and take advantage of pre-tax dollars to pay for the plan premium.
Put new technology front and center
Next-generation technology has become more important than ever in the health benefits world – and in helping sell employee benefits. Technology that improves consumer healthcare fluency, increases engagement and reduces costs will differentiate your offerings at a time when employers need good news.
The Alegeus Smart Account, now available to all 300+ Alegeus clients, exemplifies this kind of disruptor. Smart Account leverages artificial intelligence (AI) and machine learning technology to take the guesswork out of healthcare spending and saving decisions by pushing actionable insights directly to consumers. A few features on the app lead directly to cost savings for the employee, which then trickle up to the employer. The Find Care feature, for example, helps consumers choose higher-quality, lower-cost, in-network care – and can result in an 11% decrease in annual cost of care. A virtual medicine cabinet directs consumers to lower-cost prescriptions for annual savings of 16%. Simplified financial planning and investment tools analyze consumer habits and suggest savvier ways to spend and save.
These functionalities significantly increase engagement with health benefit accounts. In fact, initial data from Smart Account usage shows that two-thirds of users reengaged with the app within the first month. The stickiness of these accounts leads to more opportunities to save money. Alegeus estimates that, with Smart Account technology incorporated into the right plan design, the average consumer can save $2,289 annually on care, and a mid-sized, self-insured employer can save $600-$1,200 per employee, per year.
In addition to the cost savings, leveraging next-generation technology provides immeasurable value. A best-in-class user experience, predictive analytics, and true health and wealth convergence makes Smart Account a key tool in increasing consumer engagement and reducing service and support questions. A low-noise solution during a time of great change can be music to an employer’s ears.
Build excitement around this new approach
No one wants to sell benefits during a recession, but there’s still plenty of reason for optimism. Employers are counting on brokers and benefit administrators to deliver the encouragement – and solutions – needed to help them through this time. To make sure you deliver a winning presentation:
1. Update your sales materials.
Begin by re-architecting your sales toolkit to reflect your new value proposition. Make sure every piece sends the right message – from presentations to collateral to your website.
2. Gather feedback.
Sit down with your most trusted distribution partners to validate your approach and ask for feedback. Does your messaging hit home? Do all the pieces in your sales toolkit make sense and do their job? Is there anything you need to add?
3. Get excited!
When the time comes to give your pitch, focus on sellers and account executives within the employer group. People in these roles will be responsible for carrying your message to market. Approach the lead-up to these meetings and conversations with the excitement of a launch. To build anticipation and ensure you have full focus when walking through the solution, announce that you have a new approach to health benefits. Finally, make sure to demo any new technology during your meetings. Seeing technology firsthand will help employers visualize how their employees may engage with it.